Endometrial polyps are common, benign (non-cancerous) growths on the lining of the uterus (endometrium). They can vary in size, shape and number (from a few millimetres to several centimetres) and may appear gradually or suddenly.
Some women have no symptoms at all, with polyps discovered incidentally on an ultrasound. Others experience irregular bleeding, fertility difficulties, or postmenopausal bleeding, which can understandably cause concern.

Not all polyps cause symptoms. But if they do, you might notice some of the following:
If you’re experiencing any of these, it’s worth seeking specialist advice. Polyps are treatable, and in many cases, symptoms resolve immediately afterwards.
While the exact cause isn’t fully understood, we do know that polyps are associated with oestrogen (a hormone that stimulates the uterine lining) and inflammation. Older women (over 40), metabolic conditions, hormone treatment, and certain genetic conditions increase the risk of developing uterine polyps.

In Australia, the two most common methods are:
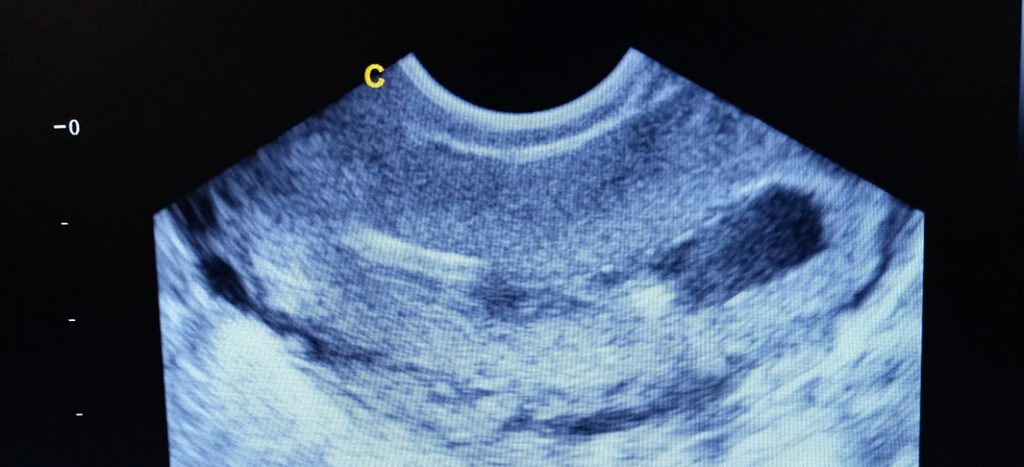
Often used as a first-line screening tool. However, polyps may be missed in up to half of cases, and it doesn’t allow for treatment.
A thin telescope inserted through the cervix into the uterus. This allows polyps to be diagnosed and removed at the same time.
Dr Tan performs both in-clinic and hospital-based hysteroscopy, depending on your preference.
Endometrial polyps are found in up to 30% of women experiencing fertility challenges or repeated IVF failure. They may:
Removing the polyp can double your chance of pregnancy, whether you’re trying naturally or through IVF.

It depends on your symptoms, age, and fertility goals.
Many polyps resolve on their own in 1–2 cycles. If you have no symptoms and are not trying to conceive, monitoring may be enough.
If you’re experiencing abnormal bleeding or fertility issues, removal is usually recommended.
Any polyp after menopause, especially if bleeding is present, should be removed because there’s a 10% chance it could be cancerous.
Dr Tan performs both in-clinic and hospital-based hysteroscopy, depending on your preference.
The most effective treatment for polyp removal is a hysteroscopic resection. This minor procedure cuts or shaves the entire polyp under vision, including its stalk, while protecting the healthy uterine lining. This reduces the chance of regrowth and preserves fertility.
In-clinic: Office hysteroscopy is a quick, well-tolerated procedure performed in private rooms without general anaesthetic thanks to special equipment and skilled techniques. Most women feel only mild cramping.
In hospital (day surgery): Under general anaesthesia if that is your preference. Recovery is usually 2–3 days.
Many women feel nervous about surgery, and that is why Dr Tan prioritises clear education and giving you choices, so that you feel informed and in control.
While polyps can’t always be prevented, recurrence can be reduced through: